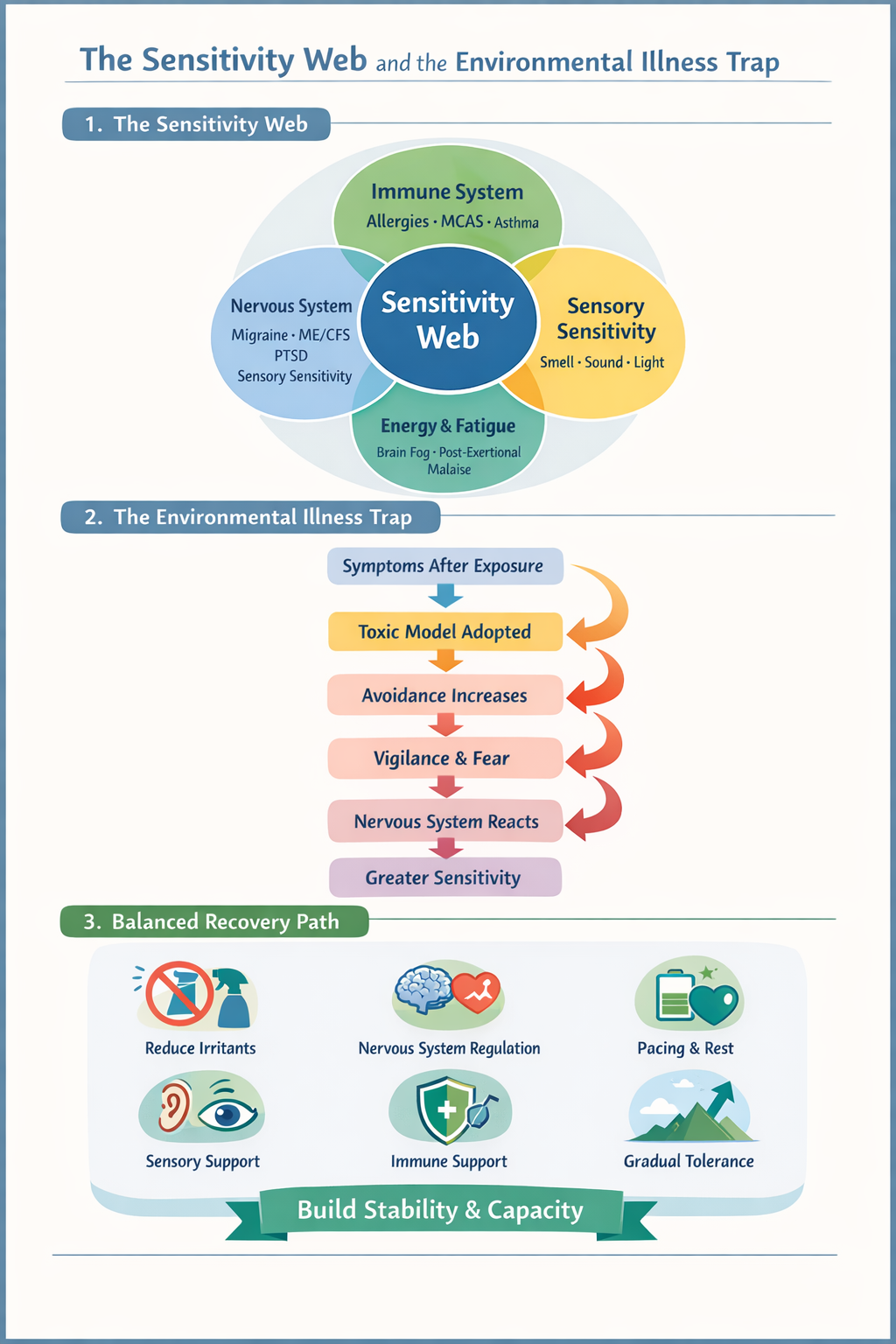
The History of the Toxic Model
The History of the Toxic Model
Environmental illness and chemical sensitivity have been described in several different ways over the past several decades. One of the earliest explanations was the toxic injury model, which proposed that exposure to chemicals in the environment could cause lasting damage to the body and lead to ongoing sensitivity to chemicals.¹
Understanding how this model developed helps explain why environmental illness remains debated in medicine today.
Early Awareness of Chemical Injury (1950s–1970s)
Long before the term environmental illness was used, doctors had recognised that high levels of chemical exposure could injure the body.
For example, workers exposed to:
- solvents
- pesticides
- industrial chemicals
- heavy metals
sometimes developed neurological symptoms such as headaches, dizziness, cognitive problems, and fatigue.²
These conditions were described as toxic encephalopathy or chemical poisoning and are well established in occupational medicine.³
Because these injuries were real and measurable, it became reasonable for some clinicians to wonder whether lower levels of exposure might also affect susceptible individuals.
The Birth of the Environmental Illness Model (1970s–1980s)
The idea that environmental exposures might contribute to chronic illness became more widely discussed in the 1970s.
One influential figure was allergist Dr. Theron Randolph, who proposed that modern chemicals in food and the environment could trigger illness in some individuals.⁴
Randolph described patients who experienced reactions to:
- perfumes
- pesticides
- food additives
- building materials
- vehicle exhaust
He suggested that repeated exposures could lead to increasing sensitivity over time.
This concept became known as environmental illness or chemical sensitivity.
Multiple Chemical Sensitivity (1980s–1990s)
By the 1980s and 1990s the condition was often called Multiple Chemical Sensitivity (MCS).
People diagnosed with MCS reported symptoms triggered by everyday exposures such as:
- fragrances
- cleaning products
- smoke
- new building materials
- fuels or solvents
Symptoms often included:
- headaches
- fatigue
- dizziness
- breathing irritation
- cognitive difficulties
Some environmental medicine practitioners believed these symptoms were caused by chronic toxic injury to the nervous system or immune system.⁵
Ongoing Debate and Research
Despite many patients reporting genuine symptoms, research findings have been inconsistent.
Controlled exposure studies sometimes showed symptoms occurring even when chemicals were not actually present but were believed to be present, suggesting that expectation and nervous system responses may also influence symptoms.⁶
Because of this, many researchers adopted the more neutral term:
Idiopathic Environmental Intolerance (IEI)
This term acknowledges symptoms related to environmental exposures without assuming a specific toxic mechanism.⁷
Different Clinical Approaches Today
Today there is no single universally accepted explanation for environmental illness, and clinicians may approach the condition in different ways.
1. Practitioners who still use the toxic injury model
Some practitioners in environmental medicine, integrative medicine, or functional medicine continue to believe that ongoing symptoms are primarily caused by toxic injury from environmental exposures.
Treatment approaches in this model may emphasise:
- strict avoidance of chemicals
- environmental controls
- detoxification protocols
- specialised diets
Some patients report benefit from reducing certain exposures, while others find that extreme avoidance can become difficult to sustain or socially isolating.
2. Practitioners who emphasise psychological explanations
At the other end of the spectrum, some clinicians believe environmental illness is primarily driven by stress or psychological factors.
This perspective may emphasise:
- cognitive behavioural therapy
- anxiety management
- gradual re-exposure to environments
This approach has also been criticised when it dismisses the real physical distress experienced by patients.
3. Emerging neuro-immune and regulation models
More recent research suggests environmental sensitivity may involve multiple interacting biological systems, rather than a single cause.
Possible mechanisms include:
• nervous system sensitisation
• autonomic nervous system dysregulation
• immune activation or mast cell responses
• sensory processing differences
Similar mechanisms are seen in conditions such as:
- migraine
- fibromyalgia
- ME/CFS
- central sensitivity syndromes.⁸
When Avoidance Becomes a Problem
While reducing harmful exposures can be helpful, some researchers caution that a strict toxic injury model may unintentionally lead to increasing fear of everyday environments.⁹
When people believe that small exposures are permanently damaging, they may begin to:
- avoid more and more environments
- restrict diet and lifestyle severely
- fear normal activities
- become socially isolated
This pattern can sometimes increase nervous system sensitivity and worsen symptoms over time.
Because of this, many clinicians now encourage balanced approaches that protect from harmful exposures while also supporting nervous system regulation and resilience.
A Balanced Understanding
Today, many researchers view environmental illness through a neuroimmune and regulation-based lens.
In this view:
Environmental triggers may be real and meaningful, but symptoms may arise from interacting body systems including the nervous system, immune system, and sensory processing.
Frameworks that focus on regulation, pacing, and load management may help people regain tolerance and stability over time.
References
Skovbjerg S et al. Idiopathic environmental intolerance attributed to chemicals. Int J Hyg Environ Health. 2012.
Ashford NA, Miller CS. Chemical Exposures: Low Levels and High Stakes. 1998.
White RF, Proctor SP. Solvents and neurotoxicity. Lancet. 1997.
Dick RB. Neurobehavioral effects of occupational chemical exposure. Occupational Medicine. 2006.
Randolph TG. Human Ecology and Susceptibility to the Chemical Environment. 1962.
Lacour M et al. Multiple Chemical Sensitivity syndrome. Int J Hyg Environ Health. 2005.
Das-Munshi J et al. Provocation studies in chemical sensitivity. J Allergy Clin Immunol. 2006.
World Health Organization. Multiple Chemical Sensitivity Workshop Report. 1996.
Yunus MB. Central sensitivity syndromes. Seminars in Arthritis and Rheumatism. 2007.