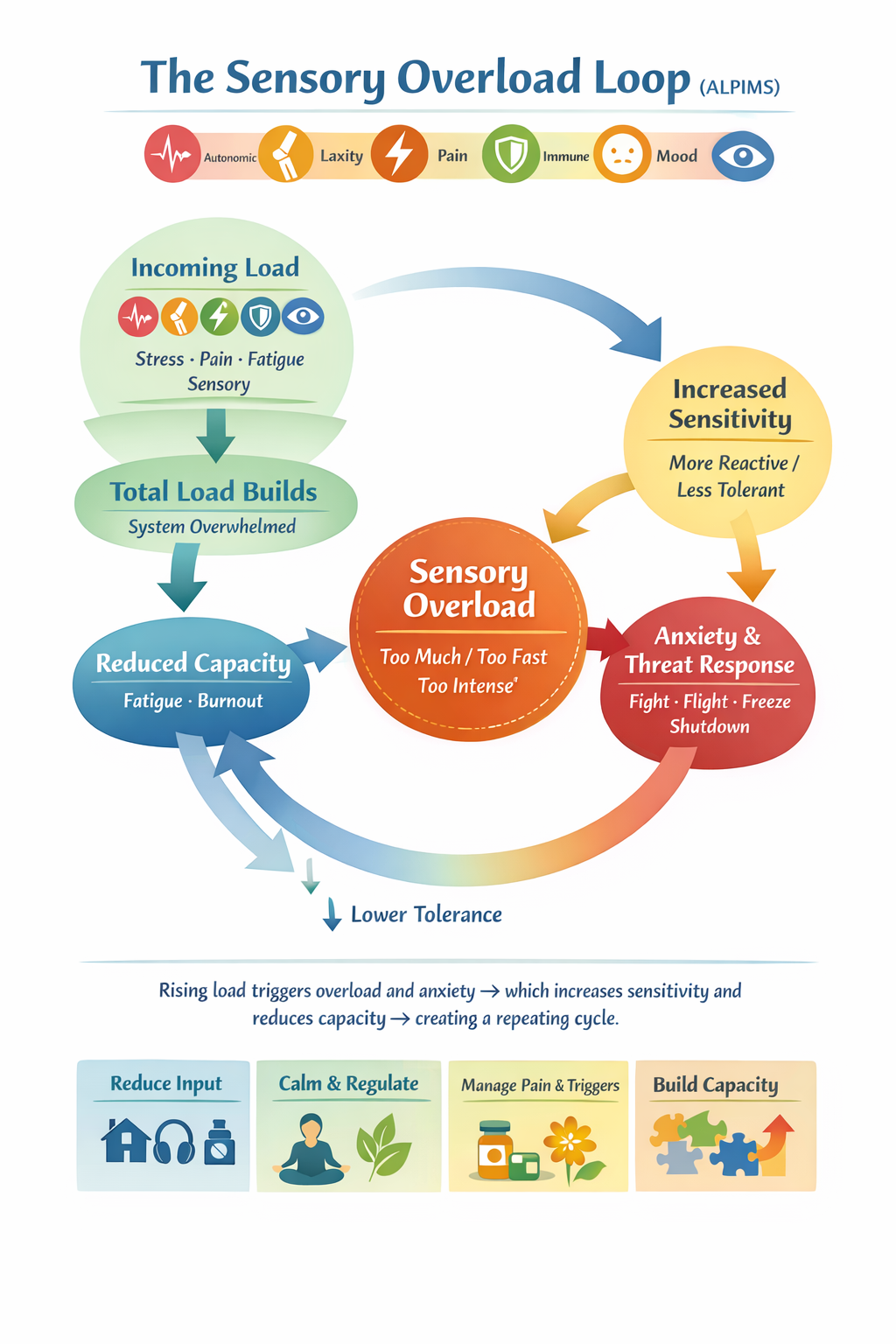
Load builds → overload → sensitivity increases → tolerance drops → repeat
This website provides educational information and personal perspectives only. It is not medical advice and should not replace consultation with qualified health professionals
References
- APA – Anxiety and stress response
- Neurodiversity and neurodivergence https://www.healthdirect.gov.au/neurodiversity-and-neurodivergence
- https://www.psychologytoday.com/au/basics/sensory-processing-disorder
- CDC – Chronic illness and nervous system regulation
- Woolf CJ – Central sensitisation
- https://my.clevelandclinic.org/health/articles/4062-chronic-illness
- Sensory Overload Wikipedia https://en.wikipedia.org/wiki/Sensory_overload
- Aspect https://www.aspect.org.au/resource-library/sensory-needs
- .Sensory Processing Disorders in Children and Adolescents: Taking Stock of Assessment and Novel Therapeutic Tools. Brain Sci. 2022 Oct 31;12(11):1478. doi: 10.3390/brainsci12111478. PMID: 36358404; PMCID: PMC9688399.