Central sensitization changes how the nervous system processes signals.
Over time, the brain and spinal cord can become more reactive to sensory input, amplifying signals that were previously manageable.
Researchers often describe the “trifecta” of central sensitization:
Hyperalgesia
Painful stimuli become even more painful than expected.
Allodynia
Stimuli that should not cause pain can become painful — such as light touch, clothing pressure, or a hug.
Global sensory hyper-responsiveness
The nervous system becomes more reactive to many types of input, including:
- Bright lights
- Loud noises
- Smells
- Foods or medications
- Internal sensations such as heartbeat or digestive movement
These patterns are commonly seen across Central Sensitivity Syndromes, including conditions such as fibromyalgia, migraine, irritable bowel syndrome, and ME/CFS.
Sometimes people with these conditions also experience symptoms associated with Functional Neurological Disorder as discussed at NHS inform.
In some people, stressful events in the past or present can be relevant to FND. Psychological conditions like PTSD, depression or anxiety can also be relevant. In other people, these things are not relevant.
The risk of developing FND increases if you have another neurological condition. It may also increase if you have a condition like autism or attention deficit hyperactivity disorder (ADHD).
The Emotional Side That Is Harder to Talk About
The symptoms are only part of the story.
Living with this kind of nervous system sensitivity often affects family life, routines, and expectations.
For many people, that brings feelings of guilt.
I have felt that too.
I worried about how my health affected my family.
I worried that the adjustments we made — quieter environments, simpler routines, certain product choices, pacing activities — might somehow take things away from them.
But when I step back and look honestly at those years, another truth is also there.
We still created joyful experiences.
We still spent time together.
We still celebrated milestones.
We still found ways to laugh, explore, and enjoy life.
Yes, we adapted some things.
But adaptation is not the same as deprivation.
When Illness Meets Family Withdrawal
Another difficult part of chronic illness is what can happen over time in relationships.
Fatigue, symptoms, and uncertainty can slowly wear people down.
Family members may become discouraged or overwhelmed.
Sometimes they withdraw.
When that happens, it can hurt deeply — especially when you know how hard you tried to hold things together.
That pain can sometimes turn into anger.
Not because you wanted conflict, but because you were already carrying so much.
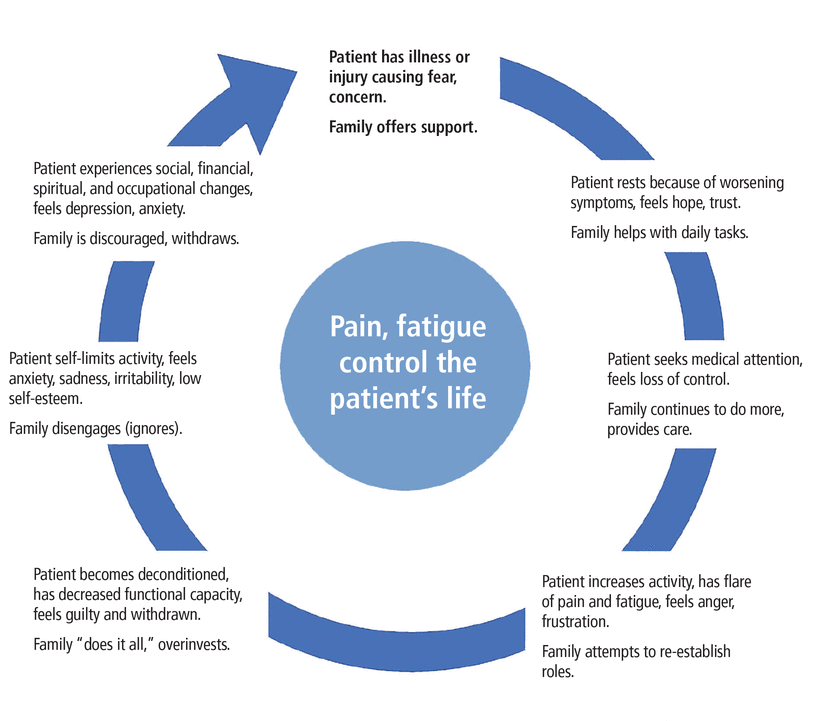
Source:https://www.ccjm.org/content/90/4/245
Looking Back with Compassion
One thing I have come to understand is this:
People navigating complex chronic illness are often doing the best they can with limited information, limited support, and an overloaded nervous system.
Families are also doing the best they can.
Sometimes everyone is exhausted.
Sometimes misunderstandings happen.
Sometimes people pull away because they do not know how to cope.
None of that erases the effort, care, and love that were present.
What I Know Now
Looking back, I know this:
I did my best to support my family while navigating a difficult health journey.
Our life included adaptations — but it also included connection, creativity, and joy.
Both things can be true at the same time.
And acknowledging that complexity is part of healing.
The following resources are recommended by the Complex Chronic Disease Program. If FND symptoms are a concern I recommend looking at NHS inform article on Functional Neurological Disorder.
Brain fog:
Sexual health:
- Sexual Health Rehabilitation Service – Blusson Spinal Cord Centre
- Sexual Health Rehab Service GF Strong Rehab Centre
Energy management:
- What is pacing (PDF)
- How to pace (PDF)
Parenting and caregiving:
- Feeding strategies and practical tips (PDF) to manage family meals when living with complex chronic diseases
- Pacing and parenting strategies (PDF) when when living with complex chronic diseases
Sleep:
Staying active:
- Manage Orthostatic Intolerance (PDF)
- Returning to physical activity (PDF)
- Exercise for Dysautonomia
- Setting Exercise Expectations for People with ME/CFS
- Gentle Movement (Pain BC)
- Heart Rate Monitoring to Stay Inside Your Energy Envelope
- Determine Your Exercise Tolerance
Work accommodations and return to work:
- Myalgic Encephalomyelitis or Chronic Fatigue Syndrome and Risk of Post Exertional Malaise from Functional Capacity Evaluations Statement Letter(PDF)
- Recommendations for Employers, Insurers, Human Resource Personnel and Rehabilitation Professionals on Return to Work for People Living with Long COVID (and Other Episodic Disabilities) (PDF)
